Understanding Compression Socks After Bariatric Surgery
Recovering from bariatric surgery requires careful attention to post-operative care guidelines. Among the various recommendations provided by medical professionals, the use of compression socks stands out as a critical component of the recovery process. These specialized garments play a vital role in preventing potentially serious complications and supporting your body as it heals and adapts to significant changes.
Bariatric procedures, including gastric sleeve surgery, involve substantial alterations to the digestive system and require periods of reduced mobility during recovery. This combination of factors increases the risk of developing blood clots in the lower extremities—a condition known as deep vein thrombosis (DVT). Compression socks provide a simple yet highly effective solution to minimize this risk and promote optimal circulation throughout the healing period.

Why Compression Socks Are Essential After Bariatric Surgery
Following bariatric surgery, your body enters a vulnerable state where blood circulation may be compromised due to limited physical activity. When you remain stationary for extended periods—whether resting in bed or sitting in a chair—blood flow in the legs naturally slows down. This reduced circulation creates an environment where blood can pool in the veins, potentially forming dangerous clots.
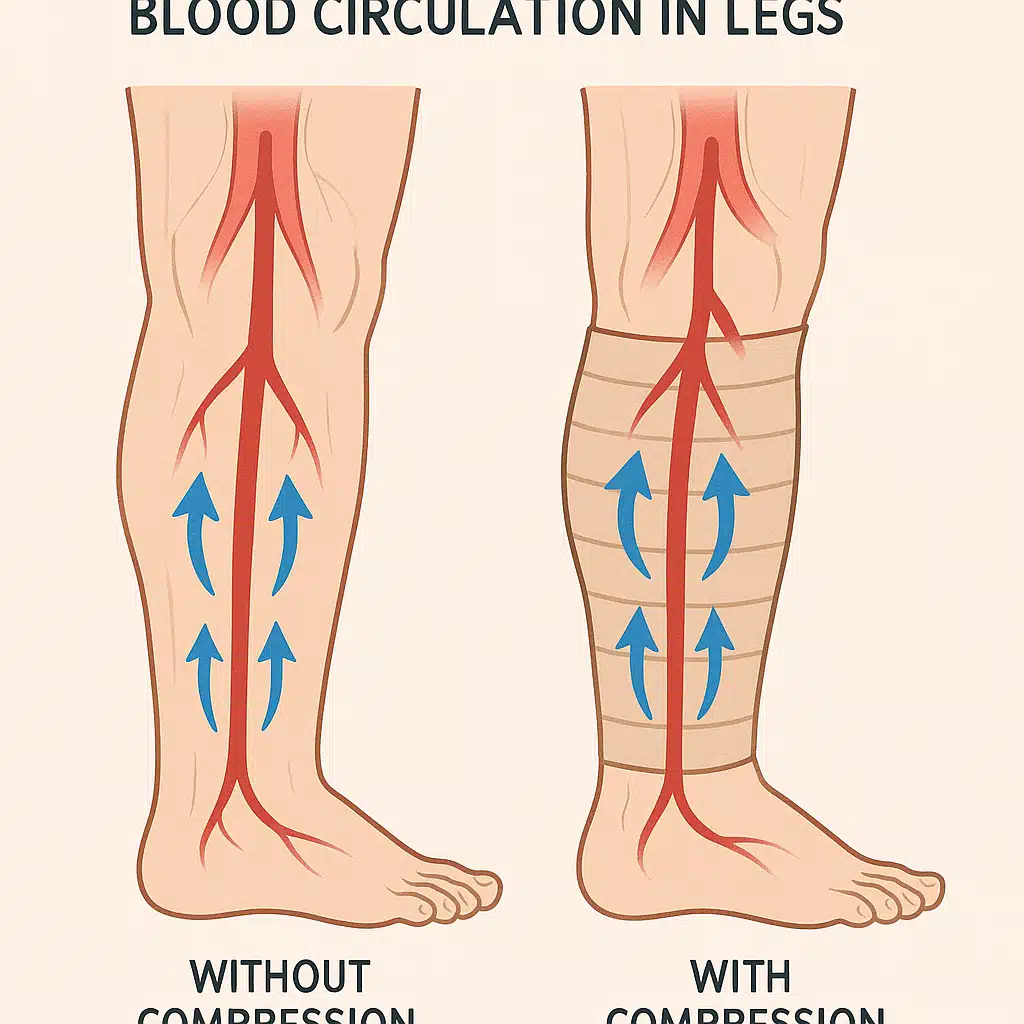
Compression socks work by applying graduated pressure to the lower legs and ankles. This gentle, controlled compression encourages blood to flow upward toward the heart, preventing stagnation in the veins. By maintaining healthy circulation, these garments significantly reduce the likelihood of clot formation.
The risk extends beyond simple discomfort. If a blood clot forms in the leg and breaks free, it can travel through the bloodstream to the lungs, causing a pulmonary embolism—a life-threatening condition that blocks blood flow to the lungs. This medical emergency can result in severe breathing difficulties and, in critical cases, can be fatal. Compression socks serve as a frontline defense against this serious complication.
How Compression Therapy Supports Your Recovery
Beyond preventing blood clots, compression socks offer additional benefits that contribute to a smoother, more comfortable recovery experience. The consistent pressure applied by these garments helps reduce swelling in the legs and feet—a common occurrence after surgery due to fluid retention and decreased mobility.
Many patients report that compression socks help alleviate the heavy, achy sensation that can develop in the legs during the post-operative period. This improved comfort level can make it easier to engage in light movement and walking exercises, which are themselves important components of recovery and clot prevention.
The physical support provided by compression garments also helps stabilize the soft tissues in your legs, which can feel particularly beneficial as you begin to increase your activity levels. This supportive function complements the circulatory benefits, creating a comprehensive approach to lower extremity health during your healing journey.
Selecting the Right Compression Socks
Not all compression garments are created equal, and choosing the appropriate type for post-surgical use is crucial for both safety and effectiveness. Medical-grade compression socks differ significantly from athletic compression wear or casual compression hosiery available in retail stores.
The key factor in compression therapy is the pressure level, measured in millimeters of mercury (mmHg). For post-surgical use, healthcare providers typically recommend graduated compression ranging from 15-20 mmHg for mild support to 20-30 mmHg for moderate compression. The term “graduated” refers to the fact that these garments apply the strongest pressure at the ankle, with gradually decreasing pressure as the sock extends up the leg—a design that optimally supports upward blood flow.

Proper fit is equally important as compression level. Socks that are too tight can restrict circulation rather than improve it, while loose-fitting garments won’t provide adequate therapeutic pressure. Your healthcare provider should take precise measurements of your leg circumference at multiple points—typically the ankle, calf, and sometimes the thigh—to determine the correct size.
Some medical professionals recommend beginning compression therapy even before surgery. This proactive approach can help establish optimal circulation patterns and may reduce risks during the surgical procedure itself. If you have pre-existing conditions such as cardiovascular disease, diabetes, peripheral artery disease, or other circulatory issues, it’s especially important to discuss compression therapy with your medical team, as special considerations may apply to your situation.
Duration of Compression Sock Use Following Surgery
The timeline for wearing compression socks varies based on individual circumstances, the specific type of surgery performed, your overall health status, and your surgeon’s protocols. However, general guidelines can help you understand what to expect during your recovery period.
Immediate Post-Operative Period (First 1-2 Weeks): During this critical initial phase, continuous use of compression socks is typically recommended. This means wearing them around the clock, including during sleep. This period presents the highest risk for clot formation due to limited mobility, anesthesia effects, and the body’s inflammatory response to surgery. Consistent compression during these vulnerable days provides maximum protection.
Transition Phase (Weeks 2-4): As you become more mobile and your body begins healing, your healthcare provider may allow you to gradually reduce wearing time. You might be advised to remove the socks for short periods—typically 2-4 hours—to allow your skin to breathe and to wash the garments. However, they should be worn throughout most of the day and often during sleep as well, unless specifically told otherwise.
Extended Recovery (Weeks 4-6 and Beyond): Many surgeons recommend continuing compression therapy for at least one month post-surgery, with some extending this recommendation to six weeks or longer. During this phase, you may be permitted to wear the socks primarily during waking hours and remove them at night. The exact duration depends on your progress, activity level, and individual risk factors.

Always follow your specific medical team’s instructions, as they understand your unique situation and can adjust recommendations based on your progress. If you experience any unusual symptoms such as increased leg pain, significant swelling, skin discoloration, or breathing difficulties, contact your healthcare provider immediately, regardless of whether you’re wearing compression socks.
Proper Technique for Wearing Compression Socks
Correctly donning compression socks ensures they function as intended and remain comfortable throughout the day. While it may seem straightforward, there’s a technique that makes the process easier and ensures proper positioning.
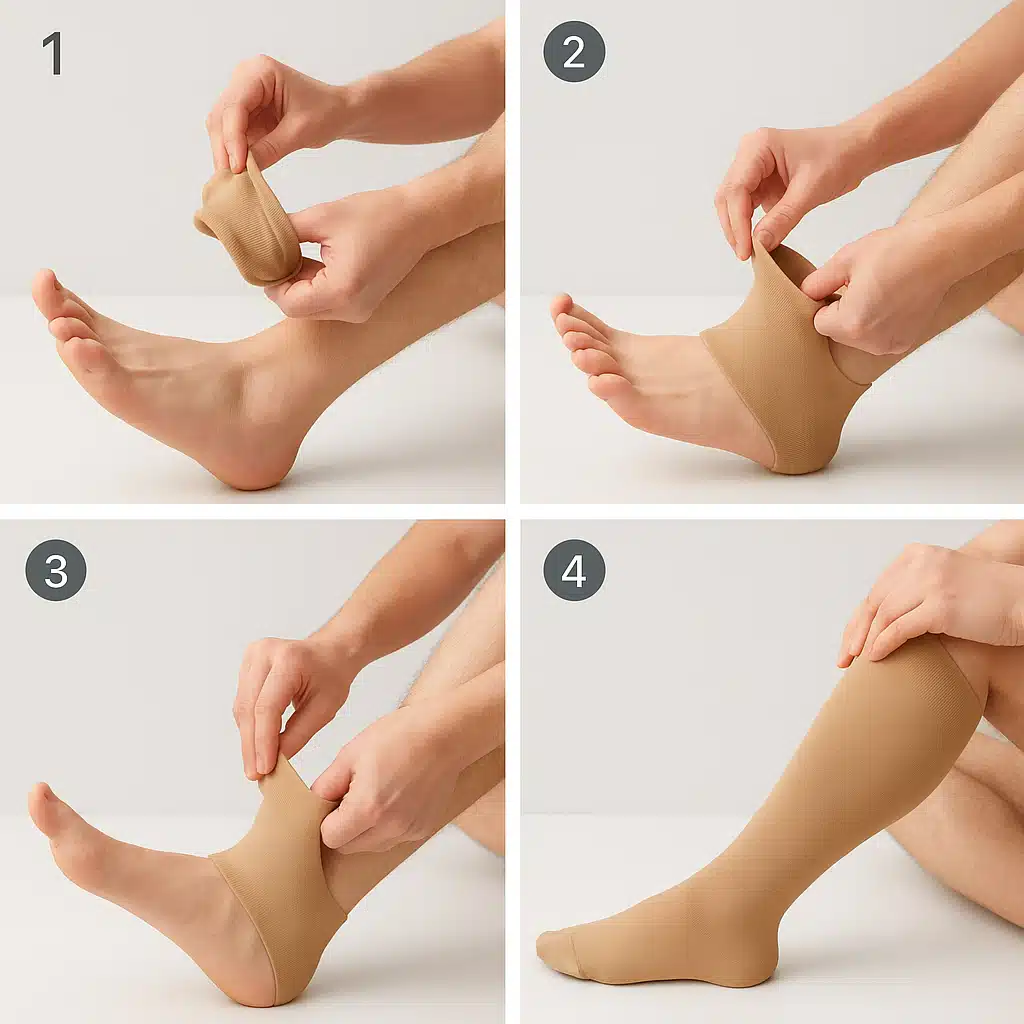
Step-by-Step Application Process:
- Prepare your legs: Begin with clean, completely dry skin. Moisture can make it difficult to pull on compression garments and may reduce their effectiveness. If you use lotion, apply it at night rather than in the morning before putting on compression socks.
- Gather the sock: Turn the sock inside out down to the heel, creating a pocket for your foot. This technique, sometimes called the “donut method,” makes application much easier than trying to pull the full length of the sock up your leg at once.
- Insert your foot: Slip your toes into the opening and position the heel portion correctly. Ensure the heel pocket of the sock aligns with your actual heel—proper positioning is essential for the graduated compression to work correctly.
- Gradually unroll upward: Slowly pull the sock up your leg, unrolling it as you go. Work in sections, using both hands to ease the material upward. Avoid tugging too aggressively, as this can damage the elastic fibers or create uncomfortable pressure points.
- Smooth and adjust: Once the sock is fully extended to the recommended height (knee or thigh, depending on the style), smooth out any wrinkles or bunched areas. Pay special attention to ensuring the top band lies flat against your skin without rolling or folding, as rolled edges can create a tourniquet effect that restricts rather than supports circulation.
- Check the fit: The sock should feel snug but not painfully tight. You should be able to slide a finger under the top band, and your toes should have adequate room to move. If you experience numbness, tingling, increased pain, or notice skin discoloration, the socks may be too tight or incorrectly sized.
Helpful Tips: Some people find that wearing rubber gloves (the type used for housework) provides better grip when pulling on compression socks. Special donning devices are also available that can make the process easier, particularly for individuals with limited flexibility or strength. Your medical supply provider can recommend appropriate accessories if you’re struggling with application.
You can wear regular shoes over compression socks, though you may need to account for the additional layer when selecting footwear. Comfortable, supportive shoes with adequate room are ideal during your recovery period.
Caring for Your Compression Socks
Proper maintenance of your compression garments ensures they continue to provide therapeutic benefit throughout your recovery period. The elastic fibers that create compression can degrade over time, especially with improper care, reducing their effectiveness.
Most medical-grade compression socks can be machine washed on a gentle cycle with mild detergent. Avoid using fabric softeners or bleach, as these products can damage the elastic fibers. Placing the socks in a mesh laundry bag provides additional protection during washing. Air drying is generally preferred over machine drying, as high heat can compromise the compression properties. If you must use a dryer, select the lowest heat setting available.
Having at least two pairs of compression socks allows you to wear one while washing the other, ensuring continuous therapy without interruption. Most compression garments maintain their therapeutic properties for approximately 3-6 months with regular use and proper care, though this can vary by quality and wear frequency.
Recognizing When to Seek Medical Attention
While compression socks are highly effective at preventing complications, it’s important to remain vigilant for warning signs that may require immediate medical evaluation. Contact your healthcare provider promptly if you experience:
- Sudden, severe leg pain or swelling, especially if limited to one leg
- Warmth, redness, or tenderness in the calf or thigh
- Unexplained shortness of breath or chest pain
- Rapid heartbeat or feeling faint
- Skin changes such as discoloration, numbness, or tingling that doesn’t resolve when you remove the compression socks
- Visible veins that become suddenly more prominent or painful
These symptoms could indicate a blood clot or other serious complication requiring immediate intervention. While compression therapy significantly reduces risk, it doesn’t eliminate it entirely, making awareness of warning signs an important part of your post-operative care.
Supporting Your Overall Recovery
Compression socks work best as part of a comprehensive recovery strategy. Early mobilization—getting up and walking short distances as soon as your medical team approves—is one of the most effective ways to prevent blood clots and promote healing. The combination of compression therapy and gentle movement creates optimal conditions for healthy circulation.
Staying well-hydrated helps maintain proper blood viscosity, making it easier for blood to flow through vessels. Following your prescribed nutritional plan, taking any medications as directed, and attending all follow-up appointments are equally important components of successful recovery.

Some patients feel tempted to discontinue compression sock use once they feel better, but it’s essential to complete the full recommended duration. The risk of clot formation can persist even after you feel you’ve recovered, making adherence to medical guidance critical throughout the entire prescribed period.
Addressing Common Concerns and Challenges
Many patients initially find compression socks uncomfortable or challenging to wear, particularly in warm weather or during sleep. These concerns are normal, and there are strategies to improve comfort while maintaining the protective benefits.
If you find the socks uncomfortably warm, look for products made with moisture-wicking materials that help regulate temperature. Keeping your living space cool, using fans, and wearing lightweight, breathable clothing can also help. Remember that any temporary discomfort is far preferable to the serious complications compression therapy helps prevent.
For those struggling with nighttime wear, try establishing a bedtime routine that includes checking the position and smoothness of your compression socks. Ensuring there are no wrinkles or twisted areas can significantly improve comfort during sleep. Some people find that elevating their legs slightly with a pillow under the calves provides additional relief.
If you have difficulty applying the socks due to limited mobility, reduced strength, or body size considerations, don’t hesitate to ask for help from caregivers or family members. Professional occupational therapists can also provide techniques and recommend adaptive equipment that makes the process more manageable.
Long-Term Considerations
For most bariatric surgery patients, compression sock use is a temporary measure limited to the post-operative recovery period. However, some individuals may benefit from continued use in specific situations. Long airplane flights, extended car trips, or periods of prolonged sitting can recreate conditions that promote blood pooling and clot formation. Many frequent travelers choose to wear compression socks during long journeys as a preventive measure.
If you have a personal or family history of blood clotting disorders, ongoing circulatory issues, or other risk factors, your healthcare provider may recommend longer-term or situational use of compression therapy. These decisions should always be made in consultation with medical professionals who understand your complete health picture.
Empowering Your Recovery Journey
Understanding why compression socks are recommended and how they protect your health can help you commit to consistent use throughout your recovery period. While they may seem like a minor detail in the larger context of bariatric surgery, these simple garments play a vital role in preventing potentially life-threatening complications.
By selecting properly fitted medical-grade compression socks, wearing them according to your healthcare provider’s instructions, and combining compression therapy with other recovery best practices, you’re taking active steps to ensure the safest, most successful outcome from your surgery. Your commitment to following post-operative guidelines, including compression sock use, demonstrates the dedication to your health that led you to pursue bariatric surgery in the first place.
Recovery is a process that requires patience, persistence, and attention to seemingly small details that collectively make a significant difference. Compression socks represent one of those important details—a simple intervention that provides substantial protection during a vulnerable time. Trust in the medical guidance you’ve been given, stay alert to your body’s signals, and know that each day of consistent compression therapy brings you closer to complete recovery and the healthier future you’re working toward.
