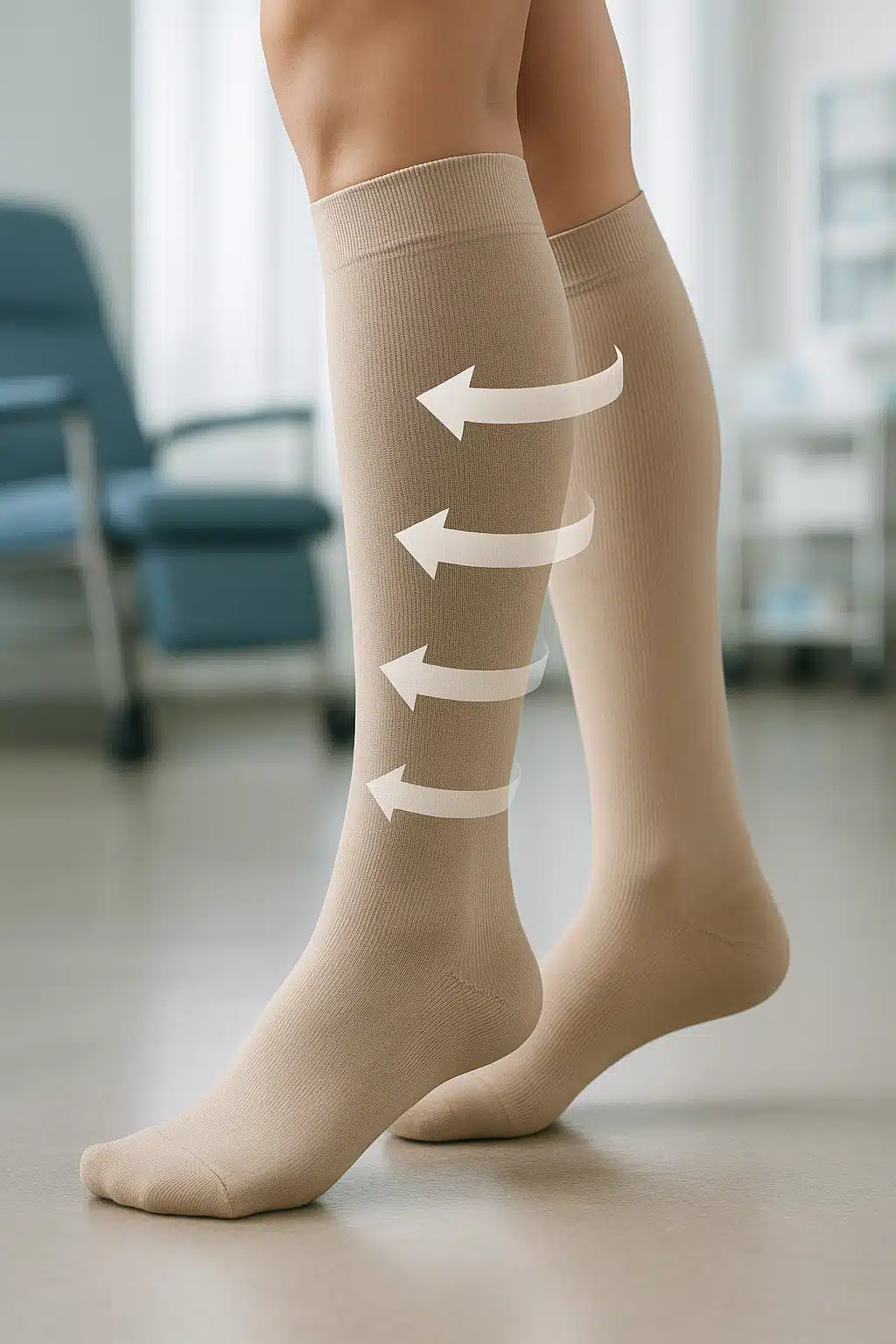
Varicose veins represent one of the most widespread circulatory concerns affecting millions of people globally. This condition develops from multiple factors including genetic predisposition, excess body weight, natural aging processes, occupational demands, and pregnancy. Common symptoms include visible swelling in the legs, persistent discomfort or pain, involuntary muscle cramping, and sensations of burning or heaviness in the lower extremities.
Among the various management strategies available, compression socks (also called compression stockings or varicose vein socks) have become a popular non-invasive option. These specially designed garments apply graduated pressure to the legs, promoting improved blood circulation and reducing venous pooling. However, compression therapy is not universally suitable for everyone, and improper use can lead to complications rather than relief.
This comprehensive guide explores the potential side effects of compression socks, identifies who should avoid them, explains proper usage techniques, and provides evidence-based recommendations to help you make informed decisions about incorporating compression therapy into your wellness routine.
What Are Compression Socks and How Do They Work?
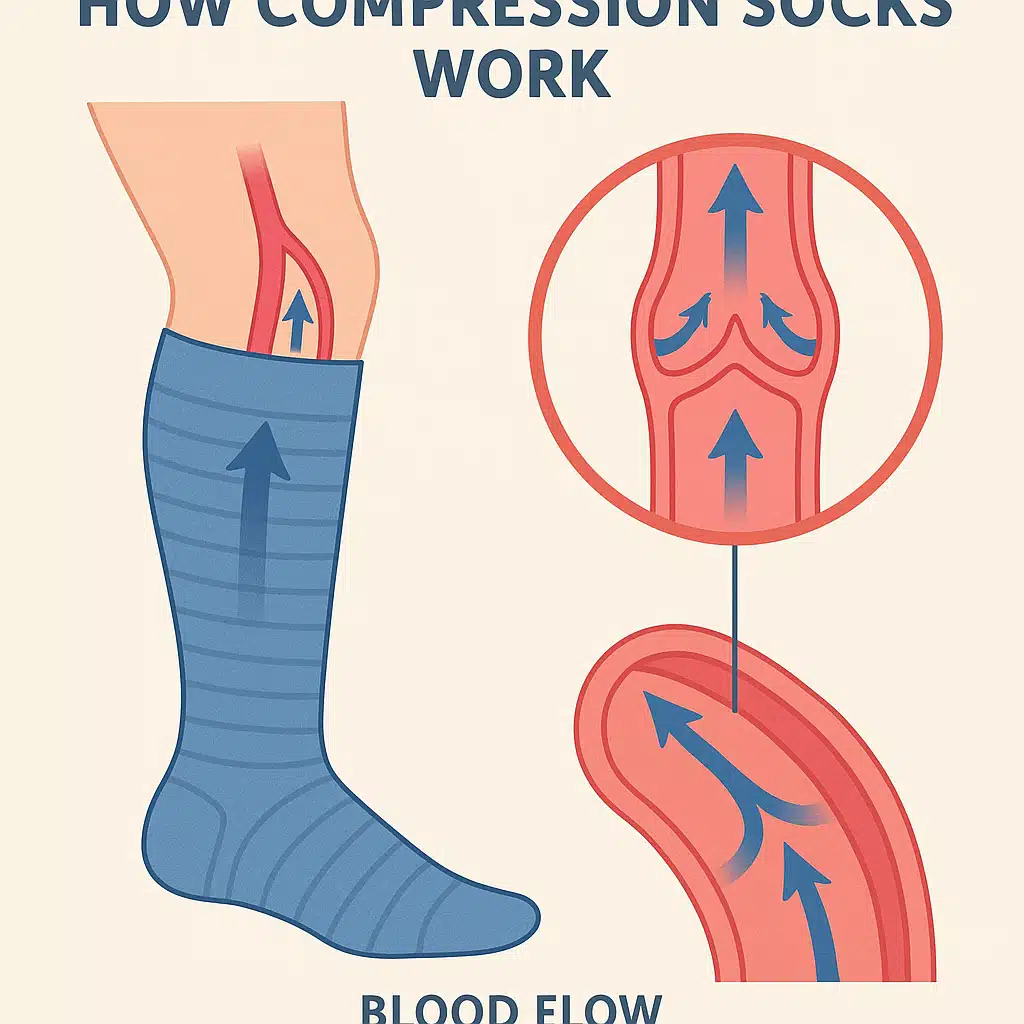
Compression socks are therapeutic garments engineered to apply controlled pressure to the lower legs and ankles. Unlike regular socks, they feature graduated compression—meaning they’re tightest at the ankle and gradually decrease in pressure as they move up the leg. This design mimics the natural muscle pump action that helps blood flow back toward the heart against gravity.
When worn correctly, compression socks help prevent blood from pooling in the leg veins, reduce swelling, improve oxygen delivery to tissues, and minimize the appearance of varicose veins. They’re commonly recommended for people who stand or sit for extended periods, frequent travelers, athletes recovering from training, pregnant women, and individuals with diagnosed venous insufficiency.
Who Should Avoid Using Compression Socks?
Before incorporating compression socks into your daily routine, it’s essential to understand that certain medical conditions and circumstances make their use inadvisable or even potentially harmful. Compression therapy works by applying external pressure to tissues and blood vessels, which can interfere with certain conditions or exacerbate existing health problems.

The following groups should exercise caution or completely avoid compression socks without explicit medical approval:
Individuals with Arterial Circulation Problems
People diagnosed with peripheral arterial disease (PAD), severe arteriosclerosis, or other conditions that restrict arterial blood flow should not use compression socks. These conditions already limit the amount of oxygen-rich blood reaching the extremities, and adding external compression can further reduce circulation, potentially leading to tissue damage or necrosis.
Those with Cardiac Conditions
Individuals experiencing congestive heart failure or pulmonary edema should consult their cardiologist before using compression therapy. In these cases, leg swelling results from the heart’s inability to pump effectively, and compression may push excess fluid into the circulatory system too quickly, potentially overwhelming the cardiovascular system.
People with Skin Conditions or Infections
Active skin infections, dermatitis, eczema, open wounds, or severe psoriasis on the legs contraindicate compression sock use. The tight-fitting nature of these garments can irritate compromised skin, trap bacteria, prevent wounds from healing properly, and spread infections to larger areas.
Individuals with Peripheral Neuropathy
Those with diabetic neuropathy or other conditions causing reduced sensation in the feet and legs face special risks. Without normal sensation, they may not recognize when compression socks are too tight, improperly positioned, or causing tissue damage, leading to serious complications before symptoms become apparent.
People with Hypersensitive Skin
Individuals prone to allergic reactions or with exceptionally sensitive skin may experience adverse reactions to the materials used in compression socks or to the constant pressure they apply. This can manifest as rashes, itching, or contact dermatitis.
If you have any chronic health conditions, have undergone vascular surgery, or are uncertain whether compression therapy is appropriate for your situation, always consult with a qualified healthcare provider before beginning use.
Common Side Effects from Improper Use of Compression Socks
Even individuals who are good candidates for compression therapy can experience adverse effects if they select the wrong size, compression level, or fail to wear the garments correctly. Understanding these potential issues helps you recognize warning signs early and take corrective action.

Discomfort and Pain
Compression socks should feel snug but never painful. If you experience significant discomfort while wearing them or sharp pain upon removal, this typically indicates that the compression level is too high for your needs or the size is incorrect. Pain is your body’s warning system—never ignore it or assume discomfort is normal or necessary for the product to be effective.
Skin Irritation and Breakdown
Excessive tightness, prolonged wear without breaks, or sensitivity to fabric materials can lead to various skin problems including redness, itching, rash formation, dry patches, or in severe cases, pressure sores. These issues often develop gradually, so regular skin inspection is important, especially during the first weeks of use.
Numbness and Tingling Sensations
If compression socks are excessively tight, they may compress nerves as well as blood vessels, leading to pins-and-needles sensations, numbness, or a feeling that your foot has “fallen asleep.” This indicates that circulation or nerve function is being compromised and requires immediate adjustment or removal of the garment.
Corns and Calluses
The constant pressure and friction from improperly fitted compression socks can create areas of thickened skin, particularly on the toes, sides of the feet, or at the top band if it’s too restrictive. These develop as the skin’s protective response to repeated irritation.
Circulation Problems from Incorrect Application
Paradoxically, compression socks meant to improve circulation can actually impede it if worn incorrectly. Common mistakes include rolling down the top band (which creates a tourniquet effect), twisting the fabric, or failing to smooth out wrinkles. These errors can cause blood to pool rather than flow properly, potentially worsening the very problem you’re trying to address.
Joint Stress
Compression socks that are too long or feature bands that sit directly over the knee joint may restrict natural movement and place abnormal stress on knee structures over time. This is particularly concerning for individuals with existing knee problems or arthritis.
Long-Term Side Effects of Excessive Compression Sock Use
While compression socks serve as an effective therapeutic tool when used appropriately, excessive or continuous use without adequate breaks can lead to longer-term complications that may take weeks or months to resolve.

Skin Changes and Chronic Dryness
Constant compression prevents normal air circulation around the skin and can interfere with the skin’s natural moisture regulation. Over extended periods, this may lead to chronically dry, flaky skin, changes in skin texture, increased fragility, or persistent discoloration. The skin of the lower legs may become thin and more vulnerable to injury.
Dependence on External Support
There is some concern among healthcare professionals that prolonged continuous use of compression garments might cause the body’s natural mechanisms for maintaining venous return to become less efficient. While this remains an area requiring more research, many specialists recommend giving your legs “days off” from compression when possible to maintain natural vascular tone.
Chronic Discomfort and Reduced Quality of Life
Some individuals who wear high-compression garments continuously report that the constant tight sensation becomes mentally burdensome over time, affecting their comfort, sleep quality, and overall well-being. Balancing therapeutic benefits with quality of life considerations is important for long-term adherence to any treatment plan.
Muscle Weakness
In rare cases, extremely prolonged use of strong compression might theoretically lead to some weakening of the calf muscle pump mechanism, as the external support partially replaces the work these muscles would normally perform. This emphasizes the importance of combining compression therapy with appropriate exercise and movement.
How to Prevent Side Effects: Best Practices for Compression Sock Use
Most side effects associated with compression socks are entirely preventable through proper selection, correct application, and appropriate usage patterns. Following these evidence-based guidelines will help you gain the benefits of compression therapy while minimizing risks.
Get Professionally Measured
Proper fit is the single most important factor in compression sock safety and effectiveness. Professional measurement, typically performed by a pharmacist, medical supply specialist, or healthcare provider, involves taking precise measurements of your ankle circumference, calf circumference, and leg length at specific points. These measurements determine your correct size and help identify the appropriate compression level for your needs.
Measurements should ideally be taken in the morning before significant swelling develops. If ordering online, follow the manufacturer’s measuring guidelines carefully, as sizing standards vary between brands.
Choose the Right Compression Level
Compression socks are classified by the amount of pressure they apply, measured in millimeters of mercury (mmHg):
- Mild compression (8-15 mmHg): Suitable for minor leg fatigue, slight swelling, or preventive use during travel
- Moderate compression (15-20 mmHg): Appropriate for minor to moderate varicose veins, mild swelling, and prevention during pregnancy
- Firm compression (20-30 mmHg): Recommended for moderate to severe varicose veins, significant swelling, and post-surgical recovery
- Extra firm compression (30-40 mmHg and higher): Reserved for severe venous conditions and requires medical prescription and supervision
Never assume that higher compression is better. Starting with excessive compression increases the risk of side effects and discomfort that may discourage continued use.
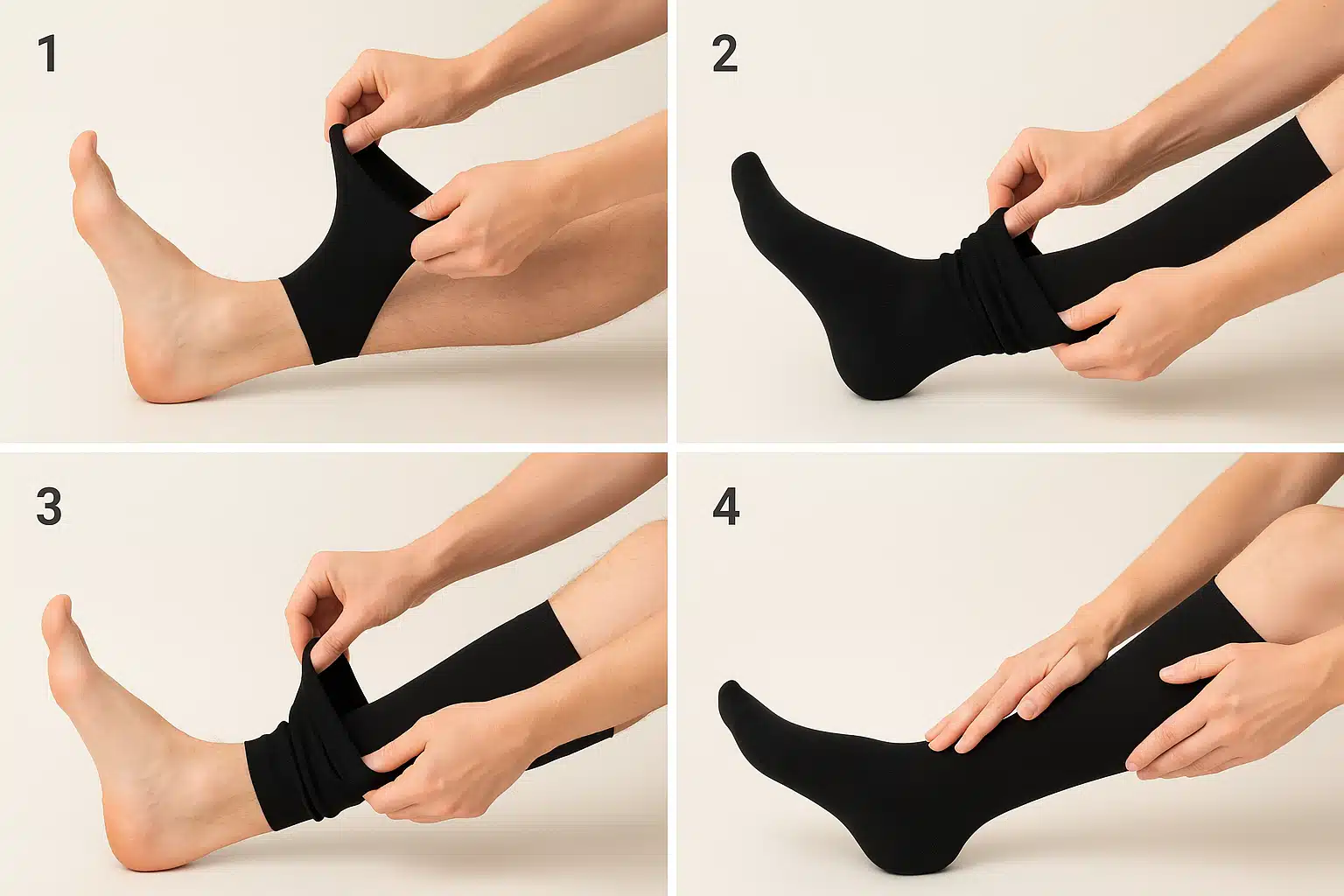
Learn Proper Application Technique
Correct application is crucial for both effectiveness and safety:
- Apply compression socks first thing in the morning before swelling develops, or after elevating your legs for 15-30 minutes
- Turn the sock inside out to the heel pocket, insert your foot, then gradually roll the sock up your leg
- Ensure the heel sits properly in the heel pocket and the sock lies smooth without wrinkles or bunching
- The top band should sit flat against your leg without rolling down or creating a tight constriction ring
- Never fold over the top or allow the sock to roll down, as this creates a tourniquet effect
- Both legs should typically be treated equally unless specifically directed otherwise by a healthcare provider
Many people find that using application aids—such as rubber gloves for better grip, metal or plastic donning frames, or silk liners—makes the process easier and helps achieve better positioning.
Follow Recommended Wearing Schedules
Compression socks are generally intended for daytime use when you’re upright and gravity works against venous return. Most healthcare providers recommend:
- Putting socks on in the morning after waking
- Wearing throughout the day during activities
- Removing before bedtime to allow your skin to breathe and recover
- Taking periodic breaks during the day if you notice discomfort
- Giving your legs complete days off from compression when feasible, especially if using higher compression levels
There are specific exceptions where overnight wear might be recommended (such as following certain surgical procedures), but this should only be done under direct medical supervision.
Maintain Your Compression Socks Properly
Proper care extends the life of compression socks and maintains their therapeutic effectiveness:
- Wash after each use using mild detergent in lukewarm water (hand washing is ideal, but gentle machine cycles are usually acceptable)
- Avoid fabric softeners, bleach, or harsh chemicals that can break down elastic fibers
- Air dry flat or hang to dry—never use a heated dryer as high temperatures damage compression materials
- Keep two pairs and alternate daily to allow complete drying and elastic recovery
- Inspect regularly for signs of wear, loss of elasticity, or damage
- Replace every 3-6 months or when they no longer provide firm support, as worn-out compression garments lose therapeutic effectiveness
Monitor Your Response
Pay attention to how your body responds to compression therapy:
- Inspect your skin daily for redness, irritation, or pressure marks that don’t fade within an hour of removal
- Note any increase in pain, numbness, tingling, or color changes in your feet or toes
- Track whether your symptoms improve, remain stable, or worsen
- Keep a journal during the first few weeks to identify patterns
- Report any concerning changes to your healthcare provider promptly
Combine with Other Healthy Practices
Compression socks work best as part of a comprehensive approach to vascular health:
- Stay physically active with regular walking, swimming, or cycling to strengthen the calf muscle pump
- Maintain a healthy weight to reduce pressure on leg veins
- Elevate your legs above heart level for 15-30 minutes several times daily
- Avoid prolonged standing or sitting—take movement breaks every 30-60 minutes
- Stay well-hydrated to maintain healthy blood viscosity
- Follow any additional recommendations from your healthcare provider

When to Seek Medical Advice
While compression socks are available without prescription in many regions, certain situations warrant professional medical evaluation before beginning use or continuing with compression therapy:
- If you have any diagnosed circulatory, cardiac, or neurological conditions
- If you develop sudden, severe, or worsening leg pain or swelling
- If you notice skin discoloration, ulcers, or wounds on your legs
- If you experience chest pain, shortness of breath, or other symptoms suggesting a blood clot
- If compression socks cause persistent pain, numbness, or skin problems
- If your symptoms don’t improve after several weeks of proper compression use
- Before using compression levels above 20-30 mmHg
Healthcare providers who specialize in vascular health include vascular surgeons, phlebologists, cardiologists, and vein specialists. Many primary care physicians can also provide initial assessment and recommendations.
Understanding the Limitations of Compression Therapy
It’s important to maintain realistic expectations about what compression socks can and cannot accomplish. They are an effective tool for managing symptoms and slowing progression of venous insufficiency, but they do not cure underlying vascular problems or reverse existing varicose veins.
Compression therapy works by mechanically supporting vein walls and valves, reducing the diameter of distended veins, and improving the efficiency of the muscle pump mechanism. This provides symptomatic relief and helps prevent worsening, but once vein valves are damaged or vein walls are permanently stretched, these structural changes typically remain.
For individuals seeking permanent treatment of visible varicose veins or experiencing severe symptoms despite compression, medical procedures such as sclerotherapy, laser therapy, radiofrequency ablation, or surgical removal may be more appropriate options to discuss with a vascular specialist.
Alternative and Complementary Approaches
While compression socks remain a cornerstone of conservative varicose vein management, they work best when integrated with other evidence-based approaches:
Exercise and Movement
Regular physical activity that engages the calf muscles—particularly walking, cycling, and swimming—naturally enhances venous return and can reduce symptoms significantly. Even simple ankle pumps and leg elevation exercises performed throughout the day help counteract gravity’s effects on leg circulation.
Dietary Considerations
While no specific diet treats varicose veins directly, maintaining healthy body weight reduces pressure on leg veins, and consuming adequate fiber helps prevent constipation that can increase abdominal pressure. Some evidence suggests that foods rich in flavonoids and antioxidants may support vascular health.
Proper Footwear
Wearing comfortable, supportive shoes with a low heel (1-2 inches) activates the calf muscle pump more effectively than flat shoes or high heels. Avoid restrictive footwear that impedes circulation.
Leg Elevation
Positioning legs above heart level for 15-30 minutes several times daily allows gravity to assist venous drainage, providing relief from swelling and discomfort. This simple technique complements compression therapy effectively.
Special Considerations for Different Populations
Pregnant Women
Pregnancy significantly increases the risk of developing varicose veins due to hormonal changes, increased blood volume, and pressure from the growing uterus. Compression socks are generally safe during pregnancy and can provide significant relief, but pregnant women should consult their healthcare provider about appropriate compression levels and duration of use.
Athletes and Active Individuals
Many athletes use compression garments during training or recovery with the belief they enhance performance and reduce muscle soreness. While research on performance benefits remains mixed, compression can help manage exercise-related leg swelling and may speed recovery. Athletic compression products typically use lower pressure levels than medical-grade compression.
Frequent Travelers
Long-distance travel, especially air travel, increases the risk of blood clots and leg swelling due to prolonged immobility and cabin pressure changes. Compression socks in the 15-20 mmHg range are commonly recommended for flights longer than four hours. Remember to also stay hydrated and perform regular leg exercises during travel.
Elderly Individuals
Older adults often benefit significantly from compression therapy but may face challenges with application due to reduced flexibility, grip strength, or vision. Donning aids, assistance from caregivers, or alternative compression devices may be necessary. Regular skin monitoring is particularly important as aging skin becomes more fragile and prone to damage.
The Future of Compression Therapy
Compression technology continues to evolve with innovations aimed at improving comfort, ease of use, and effectiveness. Recent developments include:
- Advanced fabric technologies that provide better moisture management and temperature regulation
- Seamless construction techniques that reduce skin irritation
- Fashion-forward designs that look like regular hosiery while providing medical-grade compression
- Smart compression garments with embedded sensors that monitor pressure application and wear patterns
- Adjustable compression devices that allow users to customize pressure levels throughout the day
- Improved sizing systems and made-to-measure options for better fit
These innovations aim to improve user compliance—the primary challenge with compression therapy—by addressing common barriers such as difficulty with application, discomfort, and appearance concerns.
Final Thoughts: Maximizing Benefits While Minimizing Risks
Compression socks represent a valuable, evidence-based tool for managing varicose veins and related circulatory concerns when used appropriately. The key to success lies in proper selection, correct application, and realistic expectations about what compression therapy can achieve.
Most side effects stem from preventable causes: wrong size, incorrect compression level, improper application technique, or use by individuals with contraindications. By following the guidelines outlined in this article and maintaining open communication with healthcare providers, most people can safely incorporate compression therapy into their vascular health management strategy.
Remember that compression socks are just one component of a comprehensive approach to leg health. Combining them with regular physical activity, healthy weight management, proper hydration, periodic leg elevation, and appropriate medical care when needed provides the best outcomes for long-term vascular wellness.
If you’re considering compression therapy or experiencing any concerns about your current use, consultation with a qualified healthcare provider ensures you receive personalized recommendations based on your specific health status, needs, and goals.
