Understanding Skin Structure: A Complete Guide to Skin Health and Care
The skin is the body’s largest organ, serving as a complex protective barrier between our internal systems and the external environment. Beyond defining our physical appearance, skin performs critical functions including temperature regulation, immune defense, and sensory perception. This comprehensive guide explores the scientific structure of skin, its evolution through history, and evidence-based practices for maintaining optimal skin health across all skin types and climates.
Before examining the intricate architecture of skin, it’s valuable to understand how humanity’s relationship with skin health has evolved over millennia. This historical perspective reveals how ancient wisdom and modern science converge in contemporary skincare approaches.
The Evolution of Skincare: From Ancient Remedies to Modern Science
Throughout human history, skin health has been a universal concern across cultures and continents. The journey from traditional healing to evidence-based dermatology reflects humanity’s persistent quest to understand and care for this vital organ.
Ancient Civilizations and Traditional Medicine
Early civilizations developed sophisticated understanding of botanical remedies for skin conditions. Ancient Egyptian medical texts documented treatments using natural oils, minerals, and plant extracts. Similarly, traditional Chinese medicine and Ayurvedic practices developed comprehensive systems for addressing skin health through herbal formulations and holistic approaches. These ancient practitioners recognized connections between internal health and external skin appearance—concepts that modern dermatology now validates through scientific research.
Medieval Period: Superstition and Limited Progress
During the medieval era, understanding of skin diseases regressed in many parts of the world. Supernatural explanations often replaced empirical observation, and treatments frequently incorporated mystical elements rather than therapeutic substances. This period represents a temporary setback in dermatological knowledge, though some traditional practices continued to preserve effective remedies.
Renaissance: The Birth of Scientific Dermatology
The Renaissance marked a revolutionary shift toward systematic study of skin structure and pathology. Physicians began detailed anatomical examinations and documented skin conditions with scientific rigor. This period established the foundation for dermatology as a distinct medical discipline, introducing experimental methods and evidence-based treatment approaches.
20th Century Breakthroughs
The modern era brought unprecedented advances in understanding and treating skin conditions. Pharmaceutical development produced targeted medications for previously untreatable disorders. Surgical techniques expanded treatment options for both medical and cosmetic concerns. The discovery of vitamins, antibiotics, and anti-inflammatory compounds transformed dermatological care globally.
Contemporary Era: Technology and Molecular Understanding
Today’s dermatology leverages cutting-edge technologies including electron microscopy for cellular examination, molecular biology for genetic analysis, and tissue engineering for regenerative treatments. Advanced imaging techniques allow non-invasive diagnosis, while personalized medicine tailors treatments to individual genetic profiles and skin characteristics. This integration of traditional knowledge with modern science offers unprecedented possibilities for maintaining skin health.

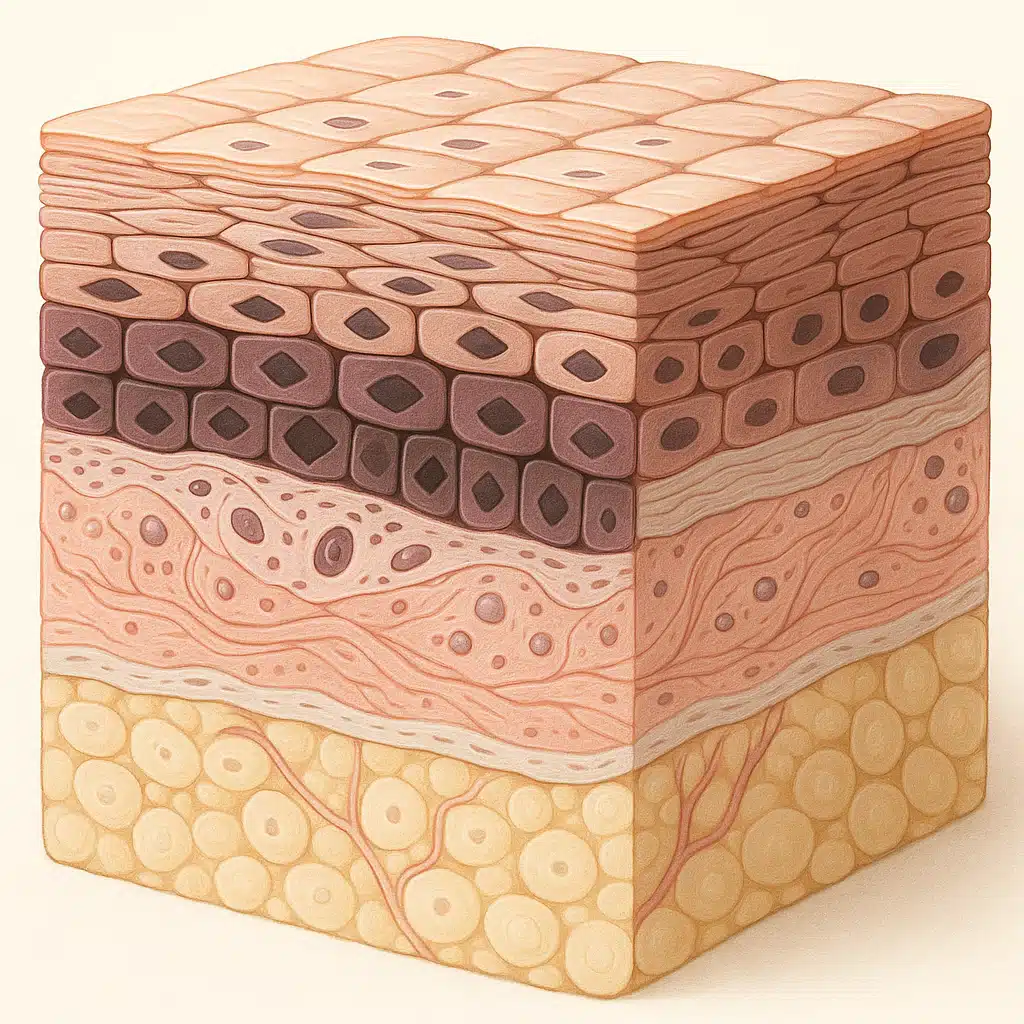
Comprehensive Anatomy: The Three Primary Layers of Skin
Human skin comprises three distinct layers, each with specialized structures and functions. Understanding this layered architecture is essential for comprehending how skin protects us and how various conditions affect different depths of tissue. The main compositional elements include structural proteins, lipids (fats), water, minerals, and an extensive network of nerve endings that enable tactile sensation. Beyond the skin itself, associated structures including hair follicles, nails, sebaceous glands, and sweat glands form an integrated system often called the integumentary system.
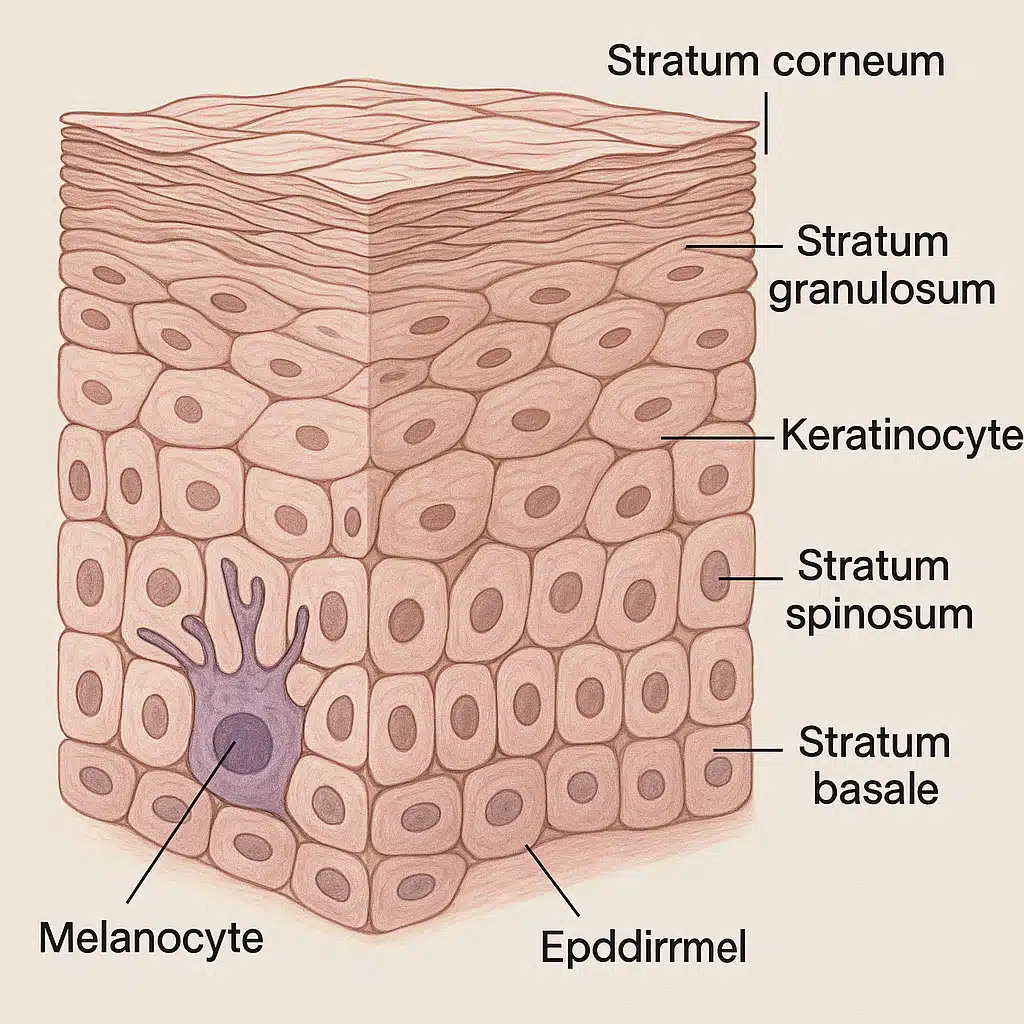
Layer One: The Epidermis (Outermost Protective Barrier)
The epidermis forms the visible surface of skin and serves as the primary interface with the external environment. This layer consists predominantly of keratinocytes—specialized cells that produce keratin, a tough protein that provides durability and water resistance. Despite being relatively thin (ranging from 0.05 to 0.1 millimeters in most areas), the epidermis performs multiple critical functions.
Many common skin conditions manifest in the epidermis, including acne, eczema, psoriasis, and various forms of dermatitis. Understanding epidermal function helps explain why these conditions present with characteristic surface symptoms.
Primary Functions of the Epidermis
- Protective Barrier Formation: The epidermis creates a waterproof seal that prevents excessive water loss while blocking entry of pathogens, toxins, and harmful substances. This barrier function is maintained through specialized lipids between cells and continuous cell renewal.
- Melanin Production and Pigmentation: Specialized cells called melanocytes produce melanin, the pigment responsible for skin color. Melanin serves a protective function by absorbing ultraviolet radiation that could otherwise damage deeper tissues and DNA. Variations in melanin concentration create the diverse range of human skin tones and affect individual susceptibility to sun damage.
- Continuous Regeneration and Repair: The epidermis completely renews itself approximately every 28-40 days through a process where basal cells divide, mature, and migrate upward, eventually being shed from the surface. This remarkable regenerative capacity allows healing of minor wounds and continuous replacement of damaged cells.
- Immune Surveillance: Specialized immune cells within the epidermis (Langerhans cells) detect and respond to potential threats, forming an important first line of immunological defense.
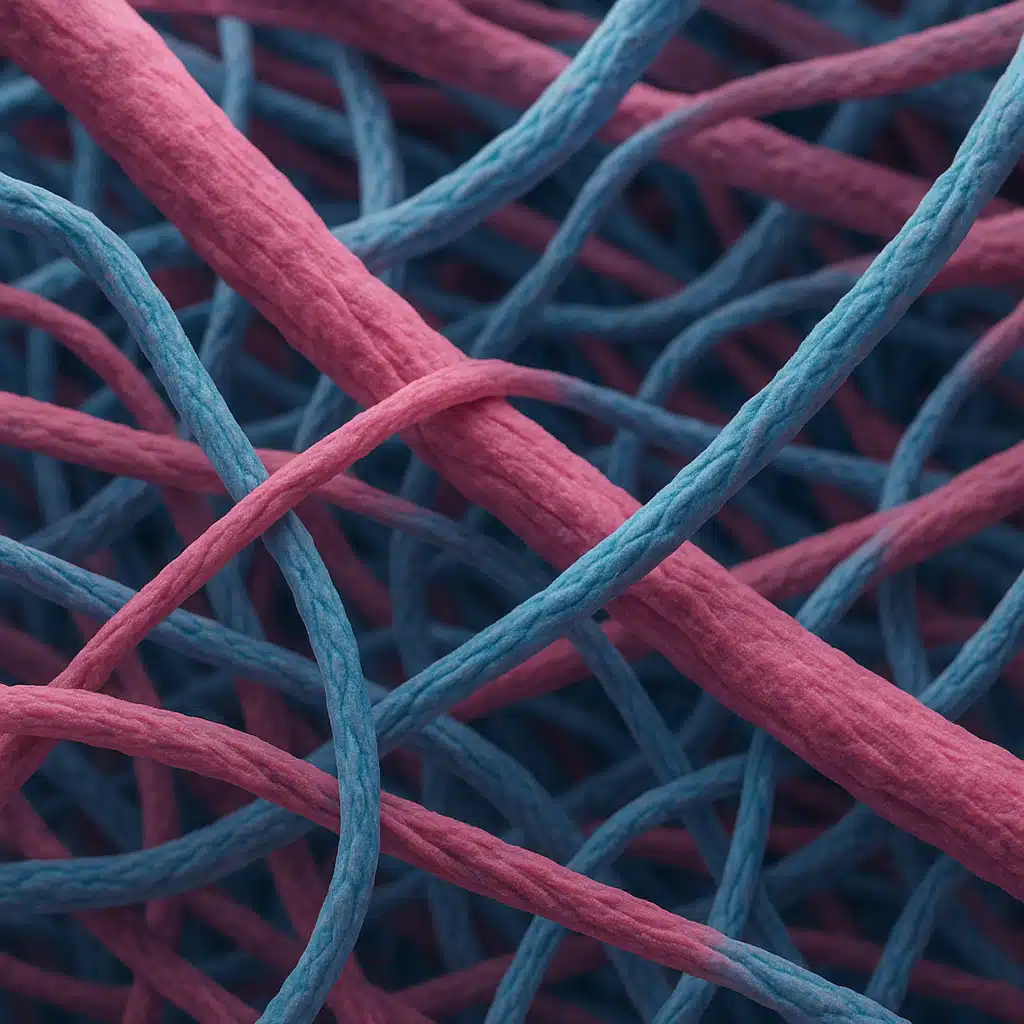
Layer Two: The Dermis (Structural Foundation)
The dermis lies beneath the epidermis and constitutes approximately 90% of total skin thickness, ranging from 0.5 to 3 millimeters depending on body location. This substantial middle layer provides structural integrity, elasticity, and houses the majority of skin’s functional components.
Two essential proteins define dermal characteristics: collagen, which provides tensile strength and firmness, and elastin, which enables skin to stretch and return to its original shape. The dermis also contains an extensive network of blood vessels, lymphatic channels, nerve endings, hair follicles, and glands.
Essential Functions of the Dermis
- Nutrient Delivery System: The dense network of blood vessels within the dermis supplies oxygen and essential nutrients to both the dermis itself and the overlying epidermis (which lacks its own blood supply). This vascular system also removes metabolic waste products.
- Sensory Perception: Specialized nerve endings and receptors in the dermis enable detection of touch, pressure, vibration, pain, and temperature changes. This sensory information allows protective responses to potentially harmful stimuli like extreme heat or cold.
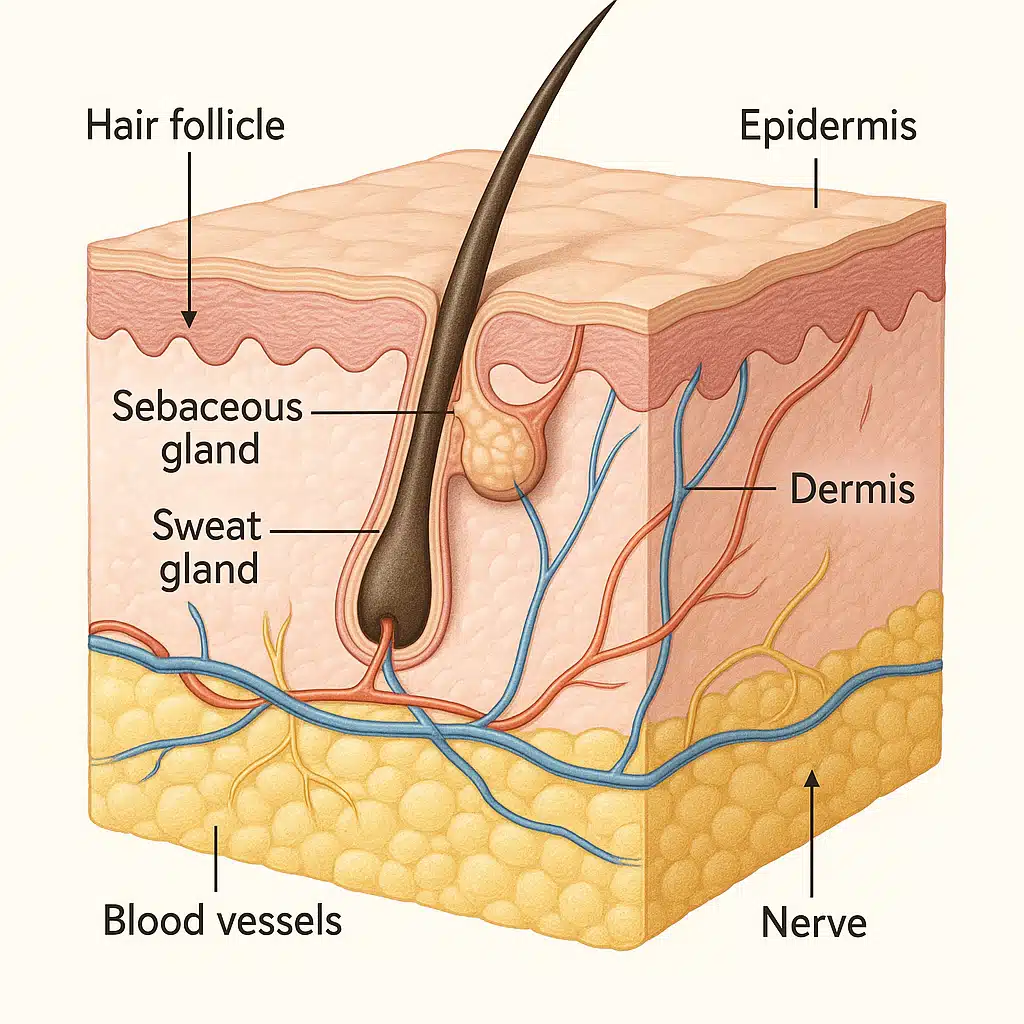
- Structural Appendages: Hair follicles originate in the dermis and extend through to the skin surface. Sebaceous glands attached to follicles produce sebum (skin oil) that lubricates and protects skin. Sweat glands regulate body temperature through perspiration.
- Mechanical Properties: The organization and density of collagen and elastin fibers determine skin’s firmness, elasticity, and resistance to mechanical stress. These properties vary with age, genetics, and environmental exposure.
- Thermoregulation: Blood vessel dilation and constriction in the dermis, combined with sweat gland activity, help maintain optimal body temperature across varying environmental conditions.
Layer Three: The Hypodermis (Subcutaneous Foundation)
The deepest layer, also called subcutaneous tissue or superficial fascia, consists primarily of adipose (fat) tissue interspersed with connective tissue. Thickness varies dramatically across different body regions and between individuals, ranging from a few millimeters to several centimeters. This layer anchors skin to underlying muscles and bones while providing cushioning, insulation, and energy storage.
Critical Functions of the Hypodermis
- Mechanical Protection: Adipose tissue acts as a shock absorber, protecting bones, muscles, and internal organs from external impacts and mechanical trauma. This cushioning function is particularly important in areas subject to pressure or friction.
- Thermal Insulation: Fat tissue provides excellent insulation against heat loss, helping maintain core body temperature in cold environments. This insulating property reduces energy expenditure required for temperature regulation.
- Structural Attachment: Connective tissue fibers within the hypodermis anchor the overlying skin layers to deeper fascial planes, muscles, and periosteum (bone covering), maintaining skin position and allowing controlled movement.
- Vascular Highway: Larger blood vessels and lymphatic channels traverse the hypodermis, connecting superficial dermal networks with deeper circulatory systems throughout the body.
- Energy Reservoir: Adipose tissue stores lipids that can be mobilized during periods of caloric deficit, serving as an energy reserve for metabolic needs.
- Endocrine Function: Fat tissue is metabolically active, producing hormones and signaling molecules that influence appetite, metabolism, inflammation, and other systemic processes.
Key Factors Influencing Skin Health and Appearance
Skin condition results from complex interactions between internal factors (genetics, age, hormones) and external influences (environment, lifestyle, skincare practices). Understanding these variables enables informed decisions about protecting and optimizing skin health throughout life.
Genetic Factors
Inherited genetic variations significantly influence fundamental skin characteristics including baseline pigmentation, thickness, oil production, sensitivity levels, and predisposition to specific conditions. While genetics establish baseline parameters, lifestyle and environmental factors modulate how these genetic potentials manifest. Understanding your genetic skin type helps tailor appropriate care strategies.
Chronological Aging
Natural aging processes affect all skin layers through multiple mechanisms. Collagen and elastin production gradually decline, leading to reduced firmness and increased wrinkling. Epidermal renewal slows, resulting in duller appearance and slower healing. Sebaceous gland activity often decreases, causing increased dryness. Fat volume in the hypodermis may diminish, contributing to hollowing and sagging. While chronological aging is inevitable, its visible effects can be significantly modified through protective measures and appropriate skincare.
Nutritional Status
Skin health directly reflects nutritional intake. Proteins provide building blocks for collagen synthesis and cell structure. Essential fatty acids maintain barrier function and reduce inflammation. Vitamins (particularly A, C, E, and D) support various cellular processes including antioxidant defense, collagen production, and immune function. Minerals like zinc and selenium participate in wound healing and protective enzyme systems. Adequate hydration maintains skin moisture and facilitates nutrient delivery. A balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats provides optimal nutritional support for skin health.
Solar Radiation Exposure
Ultraviolet (UV) radiation from sunlight represents the single most significant environmental factor affecting skin health. UVB rays primarily damage the epidermis, causing sunburn and contributing to skin cancer development. UVA rays penetrate deeper into the dermis, degrading collagen and elastin, resulting in premature aging (photoaging), hyperpigmentation, and compromised skin structure. Both UV types damage cellular DNA, increasing cancer risk. Consistent sun protection through broad-spectrum sunscreen, protective clothing, and shade-seeking behavior dramatically reduces these harmful effects regardless of geographic location or climate.
Psychological Stress
Chronic psychological stress triggers physiological responses that adversely affect skin through multiple pathways. Stress hormones like cortisol increase inflammation, stimulate oil production (potentially worsening acne), impair barrier function, slow healing, and may trigger or exacerbate conditions including eczema, psoriasis, and rosacea. Stress also often correlates with behaviors detrimental to skin health such as poor sleep, inadequate nutrition, and neglected skincare routines. Effective stress management through relaxation techniques, regular physical activity, adequate sleep, and social support benefits both psychological well-being and skin health.
Systemic Health Conditions
Many internal health conditions manifest through skin changes. Diabetes affects circulation, wound healing, and infection susceptibility. Autoimmune disorders may directly target skin components or cause secondary manifestations. Thyroid dysfunction influences skin texture, moisture, and healing capacity. Cardiovascular disease affects nutrient delivery to skin tissues. Hormonal imbalances impact oil production, pigmentation, and hair growth. These connections underscore the importance of comprehensive health management and coordination between dermatological care and treatment of underlying conditions.

Evidence-Based Skincare: Essential Practices for Optimal Skin Health
Effective skincare combines consistent basic practices with individualized approaches addressing specific concerns and skin types. The following evidence-based recommendations provide a foundation for maintaining healthy, resilient skin across diverse climates and life stages.
Proper Cleansing Techniques
Regular cleansing removes accumulated dirt, excess oil, environmental pollutants, and microorganisms without disrupting skin’s protective barrier. Choose gentle, pH-balanced cleansers appropriate for your skin type. Those with oily or acne-prone skin may benefit from twice-daily cleansing, while individuals with dry or sensitive skin often find once-daily cleansing (typically evening) sufficient, using only water or a very mild cleanser in the morning. Avoid harsh soaps or aggressive scrubbing, which can compromise barrier function and trigger inflammation. Lukewarm water is preferable to hot water, which can be drying.
Strategic Moisturization
Moisturizers serve multiple functions: they provide hydration, reinforce barrier function, reduce transepidermal water loss, and may deliver beneficial active ingredients. Apply moisturizer to slightly damp skin to seal in hydration. Select formulations matched to your skin type—lighter lotions or gel-creams for oily skin, richer creams for dry skin, and fragrance-free options for sensitive skin. Ingredients like hyaluronic acid attract and retain moisture, ceramides reinforce barrier lipids, and occlusive agents like petrolatum prevent water loss. Consistent morning and evening moisturization maintains skin hydration, comfort, and resilience.
Comprehensive Sun Protection
Daily sun protection is the single most effective measure for preventing premature aging and reducing skin cancer risk. Apply broad-spectrum sunscreen with SPF 30 or higher to all exposed skin every morning, regardless of weather or planned indoor activities, as UV radiation penetrates windows. Reapply every two hours during extended outdoor exposure, or more frequently after swimming or heavy perspiration. Complement sunscreen with protective clothing, wide-brimmed hats, and sunglasses. Seek shade during peak UV intensity hours (typically mid-morning through mid-afternoon). Many modern moisturizers and makeup products include SPF, streamlining daily sun protection.

Nutritional Support for Skin
A nutrient-dense diet supports skin health from within. Emphasize colorful fruits and vegetables rich in antioxidants that neutralize free radicals from UV exposure and pollution. Include adequate protein for collagen synthesis and tissue repair. Consume omega-3 fatty acids from sources like fish, nuts, and seeds to support barrier function and reduce inflammation. Ensure sufficient intake of skin-supporting micronutrients including vitamins A, C, D, and E, along with minerals like zinc and selenium. Maintain consistent hydration by drinking adequate water throughout the day—while individual needs vary, adequate hydration supports cellular function and helps maintain skin moisture.
Restorative Sleep
Quality sleep is essential for skin repair and regeneration. During deep sleep phases, growth hormone secretion peaks, facilitating cellular repair processes including collagen production. Blood flow to skin increases during sleep, delivering nutrients and oxygen while removing waste products. Chronic sleep deprivation elevates stress hormone levels, triggers inflammation, impairs barrier function, and accelerates visible aging. Most adults benefit from 7-9 hours of quality sleep nightly. Establish consistent sleep-wake schedules, create a comfortable sleep environment, and practice good sleep hygiene to optimize this crucial restoration period.
Stress Mitigation Strategies
Given stress’s significant impact on skin health, incorporating stress management practices provides both psychological and dermatological benefits. Regular physical activity reduces stress hormones while improving circulation that benefits skin. Mindfulness meditation, deep breathing exercises, and progressive muscle relaxation activate relaxation responses that counter stress effects. Engaging in enjoyable hobbies, maintaining social connections, and ensuring adequate personal time contribute to stress reduction. When stress becomes overwhelming, professional support from mental health providers can address underlying issues while benefiting overall health including skin condition.

Common Skincare Mistakes: What to Avoid for Healthier Skin
Understanding what not to do is equally important as knowing beneficial practices. Avoiding these common mistakes helps protect skin health and prevents unnecessary damage or complications.
Excessive UV Exposure and Tanning
Intentional tanning through sun exposure or tanning beds causes cumulative damage that accelerates aging and dramatically increases skin cancer risk. There is no such thing as a “safe tan”—visible tanning represents skin damage. Tanning beds emit concentrated UV radiation often more intense than natural sunlight, making them particularly hazardous. If you desire tanned appearance, consider sunless tanning products (self-tanners) that provide color without UV damage. Always prioritize sun protection over cosmetic tanning preferences.
Touching, Picking, and Manipulating Skin
Frequent touching transfers bacteria and oils from hands to facial skin, potentially triggering breakouts or infections. Picking at acne, extracting blackheads, or manipulating blemishes causes trauma, inflammation, and potential scarring. It can also spread bacteria, worsening existing conditions and triggering new breakouts. If you have concerns about specific skin issues, consult a dermatologist or licensed aesthetician who can perform appropriate extractions in sanitary conditions using proper techniques rather than attempting home manipulation.
Neglecting Fabric Hygiene
Pillowcases, towels, and bedding accumulate oils, dead skin cells, bacteria, and product residues that transfer back to skin during use. This microbial buildup can contribute to acne and irritation. Wash pillowcases and towels at least weekly using hot water and gentle detergent. Consider using dedicated face towels separate from body towels. Some people find that natural fiber fabrics like silk or satin pillowcases reduce friction and moisture absorption compared to cotton, potentially benefiting skin and hair health.
Harmful Lifestyle Habits
Tobacco use constricts blood vessels, reducing oxygen and nutrient delivery to skin while introducing toxic compounds that damage collagen and elastin, accelerating visible aging. Excessive alcohol consumption dehydrates skin, dilates blood vessels, and may trigger inflammation or exacerbate conditions like rosacea. Poor dietary choices—particularly diets high in refined sugars, processed foods, and unhealthy fats—promote inflammation and may worsen acne and other inflammatory skin conditions. Minimizing or eliminating these harmful exposures supports overall health while benefiting skin appearance and resilience.
Unvalidated Home Remedies
Despite widespread sharing on social media and internet forums, many popular “natural” or home skincare treatments lack scientific validation and can actually harm skin. Common problematic ingredients include lemon juice (highly acidic, causing irritation and photosensitivity), baking soda (excessively alkaline, disrupting skin pH), toothpaste on acne (containing irritating ingredients not formulated for skin), harsh physical scrubs like sugar or salt (causing microtears), and undiluted essential oils (potential allergens and irritants). Before trying any home skincare remedy, verify its safety through reputable dermatological sources or consult with a skincare professional. Well-formulated commercial products undergo safety testing and efficacy evaluation that home concoctions typically lack.

Frequently Asked Questions About Skin Structure and Care
How thick is each layer of skin, and does thickness vary across the body?
Skin thickness varies significantly depending on body location and individual factors. The epidermis typically measures 0.05 to 0.1 millimeters thick but can be considerably thicker on palms and soles (up to 1.5 millimeters) where durability is essential. The dermis ranges from 0.5 to 3 millimeters, with thicker dermis on the back and thinner dermis on eyelids and other delicate areas. The hypodermis varies most dramatically, from just a few millimeters in some areas to several centimeters in others, depending primarily on fat distribution. Factors including age, sex, genetics, and body location all influence skin thickness. Areas subject to friction, pressure, or sun exposure often develop thicker skin as a protective adaptation.
What specific roles do collagen and elastin play in maintaining youthful skin?
Collagen and elastin are structural proteins fundamental to skin’s mechanical properties and youthful appearance. Collagen, the most abundant protein in skin, forms strong fibrous networks that provide tensile strength, firmness, and structure, essentially acting as skin’s scaffolding. Elastin fibers interweave with collagen networks, providing elasticity that allows skin to stretch with movement and then return to its original position. Together, these proteins maintain skin’s smooth, firm, resilient appearance. Beginning around age 25-30, natural collagen production gradually declines (approximately 1% annually), while existing collagen and elastin fibers undergo degradation from UV exposure, oxidative stress, and enzymatic breakdown. This progressive loss manifests as wrinkles, sagging, reduced firmness, and decreased elasticity. Skincare ingredients like retinoids, vitamin C, and peptides may help stimulate collagen production or reduce degradation, while sun protection prevents UV-induced collagen damage.
How does inadequate sleep specifically affect skin health and appearance?
Sleep deprivation affects skin through multiple physiological mechanisms. During inadequate sleep, cortisol (stress hormone) levels remain elevated, promoting inflammation that can worsen inflammatory skin conditions and impair barrier function. Growth hormone secretion, which peaks during deep sleep and stimulates cellular repair including collagen synthesis, becomes insufficient with sleep deprivation. Blood flow to skin decreases, reducing nutrient and oxygen delivery while compromising waste removal, resulting in dull, lackluster appearance. Chronic sleep deprivation impairs immune function, increasing infection susceptibility. Fluid regulation becomes disrupted, often causing puffiness, particularly around eyes. Dark circles develop due to vascular changes and thin skin in the periorbital area. The cumulative effect of chronic sleep deprivation includes accelerated visible aging, compromised healing, increased sensitivity, and various inflammatory skin conditions. Prioritizing 7-9 hours of quality sleep nightly supports optimal skin repair and maintenance.
When should skin concerns prompt professional medical consultation?
While many minor skin issues resolve with basic care, certain situations warrant professional evaluation. Seek medical attention for wounds that won’t stop bleeding with direct pressure, deep wounds where edges don’t come together (potentially requiring sutures), severe burns involving large areas or showing signs of deep tissue damage, and any burns on face, hands, feet, or joints. Signs of infection including expanding redness, red streaks emanating from a wound, warmth, swelling, pus or cloudy discharge, fever, or increasing pain require prompt medical assessment. Consult a dermatologist for sudden unexplained rashes, changes in existing moles (asymmetry, irregular borders, color variation, diameter over 6mm, evolution over time), new growths, persistent lesions that don’t heal within a few weeks, severe or treatment-resistant acne, chronic conditions causing significant discomfort or affecting quality of life, and unexplained changes in skin texture, color, or sensation. Early professional evaluation of concerning changes enables timely diagnosis and treatment, potentially preventing complications or detecting serious conditions like skin cancer in early, highly treatable stages.

Conclusion: Empowering Skin Health Through Knowledge
Understanding skin’s complex structure and the factors influencing its health empowers informed decisions about daily care practices. The skin’s remarkable architecture—from the protective epidermis through the structural dermis to the cushioning hypodermis—works as an integrated system requiring thoughtful, consistent care. By implementing evidence-based practices including gentle cleansing, strategic moisturization, diligent sun protection, supportive nutrition, adequate sleep, and stress management while avoiding common mistakes, you can maintain and enhance skin health throughout life. Remember that individual skin responds uniquely to different approaches, and what works optimally may vary based on your specific skin type, concerns, and circumstances. When questions arise or concerning changes occur, don’t hesitate to consult qualified dermatological professionals who can provide personalized guidance. Your skin serves you faithfully throughout life—investing in its health through informed care delivers benefits that extend far beyond appearance to overall health and quality of life.
Important Note: This content provides educational information about skin structure and general skincare principles. It is not intended to replace professional medical advice, diagnosis, or treatment. Always consult qualified healthcare providers, particularly dermatologists, for personalized evaluation and treatment recommendations for specific skin concerns or conditions.
Scientific References and Further Reading
This article draws upon established dermatological science and evidence-based skincare principles. For those interested in deeper exploration of skin structure and care, the following reputable medical and dermatological resources provide authoritative information:
- International dermatological associations and medical institutions offering patient education about skin anatomy, physiology, and care
- Peer-reviewed dermatology journals publishing research on skin structure, aging mechanisms, and treatment efficacy
- Academic medical centers providing evidence-based information about skin health, common conditions, and preventive care
- Professional dermatology organizations offering public resources about skin cancer prevention, sun protection, and skincare best practices
