Understanding and Treating Chapped Lips: Complete Prevention and Care Guide

Chapped lips, medically known as cheilitis, is a widespread condition affecting people of all ages across the globe. It refers to dry, cracked, and sometimes painful lips that can result from environmental factors, lifestyle habits, or underlying health conditions. While chapped lips are typically a minor inconvenience, understanding their causes and learning effective prevention and treatment strategies can significantly improve comfort and overall lip health.
This comprehensive guide explores everything you need to know about chapped lips: what they are, why they occur, how to treat them, and most importantly, how to prevent them from recurring.
What Are Chapped Lips?
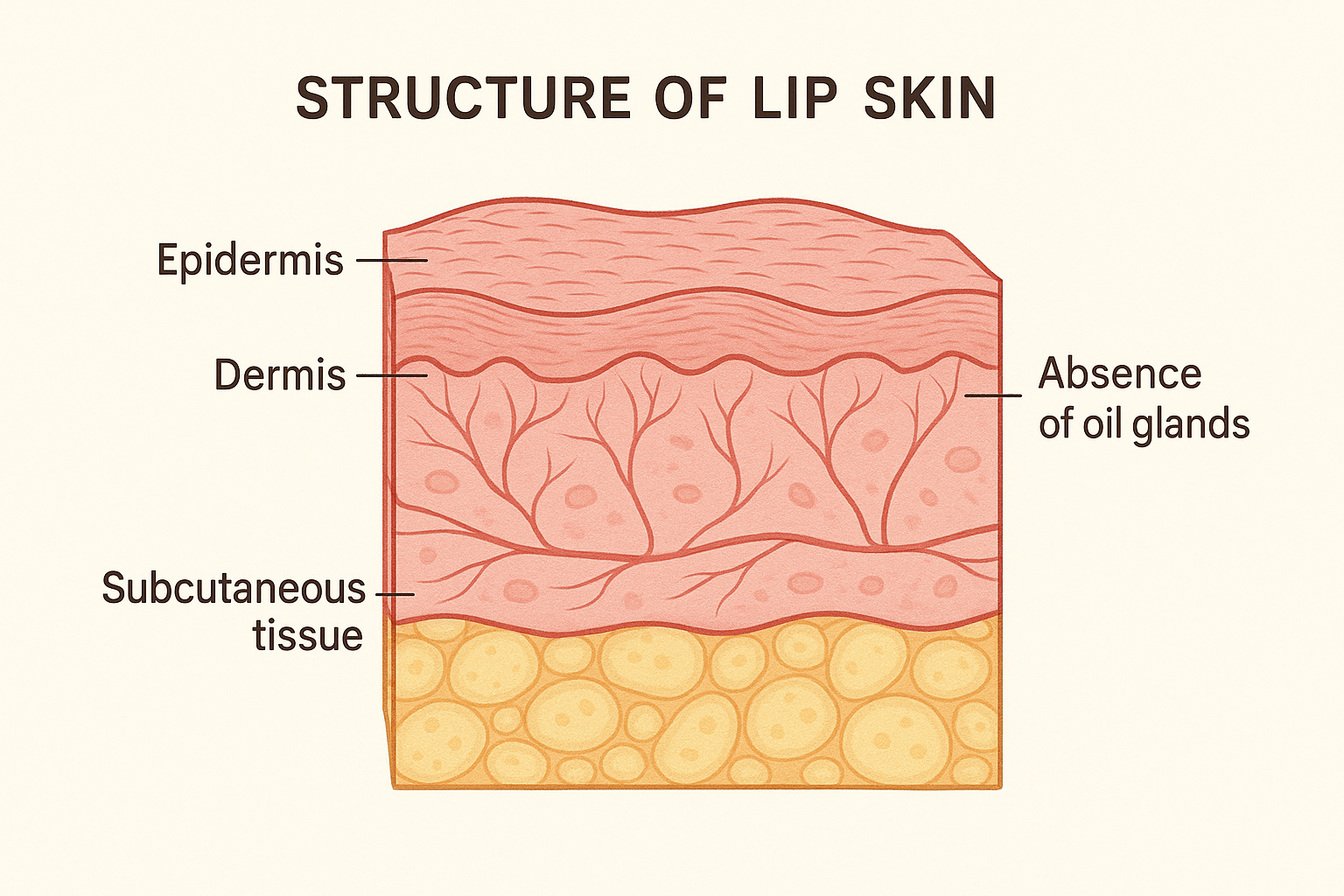
The skin covering your lips is uniquely vulnerable compared to the rest of your body. Lip skin is significantly thinner and more delicate, and unlike other areas, lips lack sebaceous (oil) glands that naturally moisturize and protect the skin. This absence of oil production makes lips especially susceptible to drying out, cracking, and becoming irritated.
Lips are constantly exposed to environmental elements—sun, wind, cold air, and indoor heating—all of which can strip away moisture. When lips lose their natural protective barrier, the result is dryness, flaking, redness, and sometimes painful cracks or splits. In more severe cases, the condition progresses to cheilitis, which may involve infection, inflammation, or cracked skin at the corners of the mouth.
Most cases of chapped lips can be managed with simple at-home care and preventive measures. However, if symptoms persist or worsen, professional medical evaluation may be necessary to rule out underlying conditions or allergies.
How Common Are Chapped Lips?
Chapped lips can affect anyone, regardless of age, gender, or geographic location. However, certain groups are more prone to this condition:
- Children and teenagers often develop chapped lips due to frequent lip licking, a habit that initially seems to add moisture but actually accelerates drying. This can sometimes lead to perioral dermatitis, a condition characterized by rashes and small red bumps around the mouth.
- People living in extreme climates—whether hot and dry or cold and windy—are at higher risk. Winter months, in particular, see a spike in cases due to low humidity and indoor heating.
- Individuals with naturally dry skin are more susceptible to seasonal or chronic chapped lips.
Understanding these risk factors can help you take proactive steps to protect your lips year-round.
Recognizing the Symptoms of Chapped Lips

Chapped lips present with a range of symptoms that vary in severity depending on the underlying cause and duration of the condition. Common symptoms include:
- Dryness or rough texture on the lips
- Flaking or peeling skin
- Visible cracks or splits in the lip surface
- Redness, inflammation, or swelling
- Itching or tingling sensations
- Mild to moderate pain, especially when opening the mouth or eating
- Sores or lesions on or around the lips
- Cracked skin at the corners of the mouth (angular cheilitis)
In more advanced cases, white patches may appear on the lip surface, or the lips may develop a lumpy texture and darker coloration. If you experience persistent or severe symptoms, it’s important to seek professional advice.
What Causes Chapped Lips?
Chapped lips can result from a wide variety of factors, ranging from environmental conditions to personal habits and underlying health issues. Understanding the root cause is essential for effective treatment and prevention.
Environmental Factors
- Cold weather: Low temperatures and harsh winds remove moisture from the lips.
- Hot, dry climates: Arid environments accelerate water loss from the skin.
- Low humidity: Indoor heating and air conditioning reduce moisture in the air, drying out lips.
- Sun exposure: UV radiation can burn and damage delicate lip skin, leading to dryness and peeling.
Behavioral Causes
- Frequent lip licking: Saliva evaporates quickly, leaving lips drier than before.
- Mouth breathing: Breathing through the mouth, especially at night, exposes lips to constant airflow.
- Picking or biting lips: These habits damage the skin barrier and worsen cracking.
- Contact with irritants: Holding objects like pens, jewelry, or metal items in the mouth can introduce allergens or irritants.
Medical and Nutritional Causes
- Dehydration: Insufficient water intake affects overall skin hydration, including the lips.
- Vitamin deficiencies: Low levels of B vitamins (especially B2 and B12) and iron can contribute to cracked lips.
- Allergic reactions: Sensitivity to ingredients in cosmetics, toothpaste, or food can trigger cheilitis.
- Medical conditions: Thyroid disorders, autoimmune diseases, eczema, and inflammatory conditions like Crohn’s disease may manifest with chapped lips.
- Medications: Certain drugs, including retinoids, lithium, and chemotherapy agents, list dry lips as a side effect.
- Infections: Fungal or bacterial infections, particularly at the corners of the mouth, can cause persistent cracking.
Identifying the specific cause or combination of causes helps tailor the most effective treatment approach.
How Are Chapped Lips Diagnosed?
In most cases, chapped lips can be diagnosed through a simple visual examination. A healthcare provider or dermatologist will assess the appearance of your lips and the surrounding skin, review your symptoms, and ask about your lifestyle, habits, and any recent changes in products or medications.
Laboratory tests are rarely necessary unless there is suspicion of an underlying condition, nutritional deficiency, or infection. If symptoms are severe or do not respond to standard treatments, further investigation may be warranted.
Effective Treatment Options for Chapped Lips

Treating chapped lips typically involves restoring moisture, protecting the lips from further damage, and addressing any underlying causes. Here are the most effective strategies:
Use Moisturizing Lip Products
Apply lip balms, ointments, or specialized lip repair products throughout the day as needed. Look for formulations containing:
- Petrolatum or glycerin for moisture retention
- Natural oils such as coconut oil, castor oil, or mineral oil
- Shea butter or cocoa butter for deep hydration
- Ceramides or dimethicone to restore the skin barrier
- SPF 30 or higher for sun protection, especially when outdoors
Apply Products Regularly
Consistency is key. Apply lip balm or ointment:
- In the morning and before bed
- Throughout the day as needed
- After eating or drinking
- Every two hours when exposed to sun or harsh weather
Adopt Protective Habits
- Avoid licking, biting, or picking at your lips
- Keep foreign objects away from your mouth
- Stay hydrated by drinking plenty of water throughout the day
- Use a humidifier indoors to maintain moisture in the air, especially during winter
Identify and Avoid Triggers
If you have a history of allergies or eczema, pay attention to potential allergens such as:
- Cosmetics, lipsticks, or lip glosses with artificial colors or fragrances
- Toothpaste or mouthwash with harsh ingredients
- Spicy or acidic foods
- Processed or preserved foods
Eliminating or reducing exposure to these triggers can significantly improve symptoms.
Treating Bleeding or Severe Cracks
When chapped lips progress to the point of bleeding, it indicates that cracks have deepened into cuts. This can be painful and increases the risk of infection. To treat bleeding lips:
- Gently clean the area with lukewarm water
- Apply a thick layer of healing ointment
- Avoid acidic, salty, or spicy foods that may irritate the area
- If bleeding persists or home remedies are ineffective, consult a healthcare professional
Risk Factors for Developing Chapped Lips
While anyone can develop chapped lips, certain factors increase susceptibility:
- Dry skin conditions: Individuals with eczema or naturally dry skin are more prone to chapped lips.
- Medications: Retinoids (including isotretinoin), lithium, chemotherapy drugs, and high-dose vitamin A supplements can cause dryness.
- Dehydration or malnutrition: Insufficient water intake or poor nutrition compromises skin health.
- Dental appliances: Braces, dentures, or retainers can increase saliva exposure to the corners of the mouth, leading to angular cheilitis.
- Age: Young children and older adults may have thinner or more vulnerable lip skin.
If you fall into any of these categories, taking preventive measures is especially important.
When to Seek Medical Attention

Most cases of chapped lips resolve with at-home care within two to three weeks. However, you should consult a healthcare provider or dermatologist if:
- Symptoms persist despite consistent treatment
- Lips become increasingly swollen, red, or painful
- You notice white patches, lumps, or unusual texture changes
- Cracks at the corners of the mouth do not heal
- You suspect an infection (indicated by pus, warmth, or fever)
- Chapped lips are accompanied by other symptoms such as fatigue, digestive issues, or skin rashes
- You experience signs of dehydration or malnutrition
A medical professional can conduct a thorough evaluation, recommend advanced treatments, and test for underlying conditions if necessary.
Choosing the Right Lip Balm
Not all lip balms are created equal. To effectively treat and prevent chapped lips, choose products with the following characteristics:
Look For:
- Fragrance-free and hypoallergenic formulations
- Ointment-based ingredients like petrolatum or glycerin
- Natural oils such as coconut, castor seed, or mineral oil
- Moisturizers like ceramides or dimethicone
- Sun protection with titanium dioxide or zinc oxide (SPF 30+)
Avoid:
- Fragrances and artificial flavorings
- Metallic compounds (some lipsticks contain lead or other metals)
- Eucalyptus or menthol, which can cause irritation
- Camphor
- Heavy waxes that may not provide adequate moisture
If a product causes tingling, burning, or worsening symptoms, discontinue use immediately.
How Often Should You Apply Lip Balm?
Lip balms and ointments work by creating a protective barrier over the lips and sealing in moisture. The frequency of application depends on the severity of your symptoms and environmental conditions:
- General use: Apply as needed throughout the day whenever you feel dryness.
- Before bed: A generous application at night helps lips heal while you sleep.
- After meals: Reapply after eating or drinking to maintain protection.
- Outdoor activities: Reapply every two hours when exposed to sun, wind, or cold weather.
Keep lip balm easily accessible—carry it in your bag, keep it on your bedside table, and store one in your car for convenience.
Preventing Chapped Lips: Long-Term Strategies

Prevention is always better than treatment. By incorporating simple habits into your daily routine, you can keep your lips healthy and avoid the discomfort of chapping:
- Daily lip care: Apply lip balm with SPF every morning and reapply throughout the day.
- Nighttime routine: Use a thick, nourishing ointment before bed.
- Hydration: Drink plenty of water to maintain overall skin moisture.
- Humidify your environment: Use a humidifier in your home, especially during dry seasons.
- Protect from the elements: Wear scarves or face coverings in cold, windy weather and apply SPF lip balm before sun exposure.
- Avoid irritants: Choose gentle, hypoallergenic personal care products.
- Maintain a balanced diet: Ensure adequate intake of vitamins and minerals, particularly B vitamins and iron.
What to Expect During Recovery
With proper care, most cases of chapped lips improve significantly within a few days to two weeks. Severe cracking or cheilitis may take longer—up to three weeks or more—to fully heal. Prompt treatment at the first sign of dryness accelerates recovery and helps prevent complications such as infection or chronic inflammation.
In general, chapped lips are a harmless condition that causes temporary discomfort. However, if symptoms persist or worsen despite treatment, it may indicate an underlying medical issue that requires professional evaluation.
Why Some Chapped Lips Don’t Heal
If your chapped lips do not improve with standard care, several factors may be at play:
- Underlying health conditions: Thyroid disorders, autoimmune diseases, or inflammatory conditions may require targeted treatment.
- Persistent allergen exposure: Continued use of products containing irritants or allergens prevents healing.
- Nutritional deficiencies: Low levels of essential vitamins and minerals impair skin repair.
- Infection: Bacterial or fungal infections need medical treatment with appropriate antimicrobial agents.
- Medication side effects: Some drugs cause chronic dryness that may require adjustment or supplementary treatments.
If your lips remain stubbornly dry, cracked, or painful despite diligent care, consult a healthcare provider. They can conduct tests, adjust medications, or prescribe more advanced treatments to address the root cause.
Final Thoughts
Chapped lips are a common, usually minor condition that can cause discomfort and embarrassment. Understanding the causes—from environmental factors to lifestyle habits and underlying health issues—empowers you to take effective action. With the right combination of moisturizing products, protective habits, and attention to potential triggers, you can keep your lips soft, healthy, and comfortable year-round.
Remember to stay hydrated, protect your lips from harsh weather, and choose high-quality lip care products suited to your needs. If symptoms persist or worsen, don’t hesitate to seek professional guidance. Your lips are an important part of your overall health and appearance, and they deserve the care and attention necessary to stay in optimal condition.
